Issue 3.2
Editorial – Alberto Mazzocchi MD, DDS (VJO associated editor)
In the last issue of VJO you will find a clinical article on Indirect Bonding. We tested a new improved adhesive made by 3M Unitek tm. Though resins and adhesives are constantly improving, there is no consensus on the indirect bonding technique. It is safe to say that many orthodontists think that this is a terrific technique but only a few of them actually use it. The question is why? Indirect bonding allows precise bracket placement. Positioning brackets on a model is obviously easier since the crown inclination or rotations can easily be checked without bothering the patient. It is a lot more convenient to control roots looking at X rays in one hand and models on the other hand. Everyone can visualize perfect bracket placement even on first or second molars. Cleaning of resin is easier around the brackets and one can use the correct amount of composite on casts without wasting one’s time with scalers or handpieces in the patient’s mouth. Finally it is possible to do a full bonding in 10 minutes. Orthodontists who are reluctant say that they can place brackets with…….
Skeletal Distraction for Mandibular Lengthening with a Completely Intraoral Toothborn Distractor (English – Italian – Spanish)
Yan Razdolsky D.D.S.
Abstract: Distraction osteogenesis is the process of generating new bone by stretching (intramembranous histogenesis).
In 1905, Codvilla described the concept of osteodistraction1. Technical problems associated with distraction of long bones were later circumvented by several investigators, most notably, Ilizarov and DeBastiani, 102 McCarthy et al. in 1992 first described distraction of the hypoplastic mandible in humans.
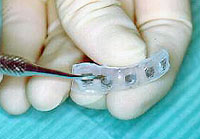
The deficiencies that distraction addresses are not isolated to the skeleton but affect the soft tissues, including the skin, musculature and neurovascular structures. As our experience with this technique for correction of facial deformation has expanded we have modified our management of patients presenting with skeletal and soft tissue deformation of the face. Our initial experience with osteodistraction utilized external fixators to achieve bone and soft tissue elongation. Disadvantages of the procedure were the presence of external scars and the requirement that patients wear a cumbersome device for approximately 8 weeks. In order to circumvent the previous limitations of osteodistraction of the mandible we have developed a distraction device which is totally intraoral and completely toothborne! This report comprises our initial experience with the intraoral and completely toothborne device.
PROSTHETIC REHABILITATION FOR PATIENTS WITH LABIOPALATOSCHISIS: traditional and new approach (English – Italian – Spanish)
Roberto Branchi MD, DDS
Abstract: The prosthetic treatment of labiopalatoschisis (L.P.S.) is the final step of a long procedure involving orthopaedic surgery of the maxilla, reconstructive plastic surgery, and orthodontic treatment. Patients are usually referred to the prosthodontist at age 14 to replace missing teeth in the schisis area. The purpose of this article is to show a clinical case followed from the age of 14 to 27.
INDIRECT BONDING a new improved adhesive (English – Italian – Spanish)
Alberto R. Mazzocchi MD, DDS
Abstract: Though fewer than 20% of orthodontists use an indirect bonding technique (5), there is general agreement that brackets can be positioned more accurately extraorally on a study model than intra-orally on teeth. This statement is even more important when it comes to using pre-adjusted brackets. Indirect bonding offers significant rewards in term of quality of care and efficiency of treatment.
Orthodontic treatment conceptions (fourth part)
(According to McLaughlin-Bennet -Trevisi)
Arturo Fortini MD, DDS
Massimo Lupoli MD, DDS
Le Disfunzioni del Sistema Cranio-Cervico-Mandibolare (quarta parte)
Umberto Montecorboli MD, DDS